Tendon injuries are often automatically slapped with the label “tendonitis,” yet the real problem is much more likely to be “tendinosis.” Regardless of your fitness pursuits, understanding the distinction can dramatically alter your treatment and speed your recovery.
The difference is fairly simple: Tendonitis (as the “itis” suffix suggests) involves tendon inflammation; tendinosis describes tendon degeneration without inflammation. Both fall under the more general umbrella diagnosis of “tendinopathy,” but nearly all cases of tennis elbow, sore Achilles’ tendons, jumper’s knee, shoulder pain and foot problems stem from tendinosis. Instances of tendonitis, on the other hand, are relatively rare.
What Is Tendonitis?
Tendonitis is caused by the rapid convergence of white blood cells on an injured tendon, provoking an inflammatory reaction. Normal tendon strands lie side by side, but when suffering from tendonitis, they swell and bump against each other. The injured area is warm to the touch and can be quite painful.
Tendonitis shows up white on an MRI.
Luckily, with a little ice and rest, tendonitis takes as little as two weeks to heal, says Scott Rodeo, MD, an orthopedic surgeon and clinician-scientist at The Hospital for Special Surgery in New York, as well as a team doctor for the 2007 Super Bowl champion New York Giants.
(Additional characteristics of tendonitis.)
What Is Tendinosis?
Tendinosis, on the other hand, stems from chronic overuse rather than a single acute event. “With tendinosis, there’s an abnormal collagen or protein buildup — the tendon’s microfibers start to resemble sticky, overcooked spaghetti,” says Karim Khan, MD, PhD, assistant professor of family medicine and human kinetics at the University of British Columbia in Vancouver and coauthor of Clinical Sports Medicine.
Damage occurs at a microscopic level long before symptoms of pain, tightness and soreness appear. As with tendonitis, you might feel anything from a slight twinge to a jabbing pain.
Tendinosis shows up black on an MRI.
Tendinosis usually occurs because you have not rested enough between workouts that require heavy or stressful loading to the affected area. But, because researchers have not specifically identified an optimal rest period to prevent the condition, many fitness experts simply recommend that you follow a periodized program, with built-in deloading phases, to help prevent such overuse injuries. Cross-training can also help you avoid overusing a particular area.
Unlike tendonitis, tendinosis often requires at least three to six months for recovery. “It’s not realistic to think you can heal in, say, six weeks, because it probably took a lot longer than that to reach the point of pain,” says Bryan Chung, MD, PhD, founder of the blog Evidence-Based Fitness (www.evidencebasedfitness.blogspot.com).
Some physicians even stretch that recovery period to nine months or more. Tendinosis takes a considerable amount of time to heal because of limited blood flow to tendons, and because it can take 100 days for your body to reestablish strong collagen, which repairs damage.
(Additional characteristics of tendinosis.)
How to Recover from Tendinosis or Tendonitis
The good news: You don’t have to be inactive during your recovery. In fact, inactivity can actually slow tendinosis recovery. Following the right treatment plan can encourage your tendon to reconstruct itself with healthy, normal tissue.
“You’ll want to scale back your usual routine or pursue alternative activities,” says Chung. “If you’re a runner, for example, you might hop on the exercise bike or do some water running instead. But total abstinence is probably not a great idea because you’re likely to fall behind on your overall fitness goals.” And that, the experts note, can make it tougher for you to come back from your injury. (For more ideas about moderating activity, see “How to Exercise With Knee and Hip Pain.”)
Inactivity can actually slow tendinosis recovery.
Often, effective treatment plans include eccentric exercises, which focus on the “negative” component of a movement. And for good reason: A 2004 study conducted by the University of Umea in Sweden indicated that eccentric exercises speed collagen rebuilding.
Khan recommends eccentric exercises such as heel drops for Achilles’ tendinosis, mini-squats for jumper’s knee and wrist drops for tennis elbow. (For more on eccentrics, see “What Is Eccentric Training?”)
While researchers can’t definitively explain how eccentrics heal, the theory, explains Khan, is that our bodies send something called “neovessels” to the site of the injury, which impede the healing process and stimulate nerve endings, causing us to feel pain. Eccentric training effectively kills off those neovessels, thus promoting healing and reducing pain.
Treatments for Tendon Health and Recovery
The best route for treatment, of course, depends on the individual, but healthcare professionals agree that ibuprofen and the other non-steroidal anti-inflammatory drugs (NSAIDs) often recommended for tendonitis symptoms don’t relieve tendinosis because there’s no inflammation present. They could even impair healing.
Equipment modification, however, can make a difference, says Allan Mishra, MD, an adjunct orthopedic surgeon at Stanford University. “Ill-fitting shoes can be an issue, and in the case of tennis elbow, the grip on your racket might be too small or too big,” he explains. “Your computer keyboard might also be a problem. Basically, anything that involves gripping, twisting or bending can lead to tendon injury.”
In addition to correct-fitting equipment, a personalized, therapeutic stretching program is a must, says Mishra. Other treatments include acupuncture, ultrasound, deep-tissue massage, and electronic muscle stimulation. All of these treatments are designed to increase the supply of blood and its collagen-rebuilding element to the tendon and affected area. This is especially critical for shoulders and elbows, parts of the body where blood supply is relatively poor.
If patients show no improvement after six months of a specialized strength and stretching program, physicians sometimes consider using nitric-oxide patches (used for heart-disease patients but showing promise with tendon repair), cortisone injections or even surgery. Mishra, for his part, is testing new platelet-rich plasma injections in clinical trials.
But the preferred treatments remain noninvasive. “Our bodies have the power to heal within,” says Mishra. “That’s the best way.”
ITIS vs. OSIS
On his Web site www.bodybuilding.com, David Ryan, MD, compares the characteristics of tendonitis and tendinosis this way:
Tendonitis
- Shows up white on an MRI
- Inflammatory
- Very rare
- Requires only 14 days to heal
- Aggravated by exercise
- Usually warm to the touch
- Loves ice and rest
- Not helped by friction massage
- Helped by NSAIDs
- Irritated by heat
Tendinosis
- Shows up black on an MRI
- Degenerative
- Very common
- Requires months to years to heal
- Treated with therapeutic exercise
- Usually cool to the touch
- Not helped by ice and rest
- Helped by friction massage
- Irritated by NSAIDs
- Responds to electric stimulation and heat
Illustrations of Tendons
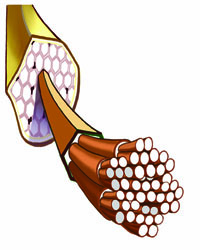
Healthy Tendon
The tendon has smooth “strands” that lie side by side.
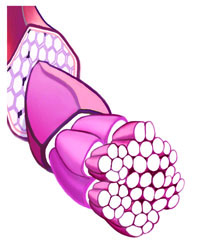
Tendonitis
The strands are inflamed, looking bloated and puffy. A magnetic resonance imaging (MRI) test will show a lot of white, which indicates inflammation.
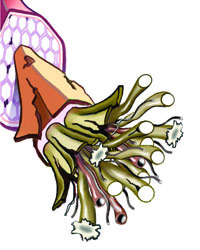
Tendinosis
The strands are twisted, scarred, shortened and otherwise degenerated. This tissue, which requires three to nine months to completely regenerate, appears black on an MRI.
Say No to NSAIDs?
Most doctors discount non-steroidal anti-inflammatory medications (NSAIDs) for healing tendinosis, mainly because no inflammation is present with tendinosis. New York Giants team physician Scott Rodeo has presented lectures on the theory that NSAIDs might even disrupt healing in your injured tendon. Studies conducted at the University of North Carolina indicated that the NSAIDs block production of DNA that would otherwise be creating genetic material to rebuild smooth, healthy tendon microblast fibers.
If pain is an issue, try acetaminophen or Tylenol — or consider acupuncture, which may offer pain relief and speed healing. Icing can also numb the area before or after activity without any longer-range hindering of DNA repair to the tendon.
This article has been updated. It was originally published in the May 2008 issue of Experience Life.




This Post Has One Comment
I developed what my medical pros thought was Achilles tendonitis in my left foot last August. I went to a physical therapist twice a week and did all the home exercises they taught me faithfully, but my symptoms did not subside. After four months, I quit going to physical therapy because I was not making any progress, but I continued the home exercises on my own for two months. Still no improvement. Then, a friend of mine, a retired doctor, suggested I see a PT she knew to be an expert in foot issues. That new PT made orthotics for me which helped me a bit, and taught me new exercises that were eccentric. She also suggested an Orthopedic surgeon to me. I received a referral from my PCP and made an appointment with her but I couldn’t see her for two more months. She suggested that I receive an MRI, for which I waited another 6 weeks.
The MRI revealed some tears in my Achilles tendon which the doctor diagnosed were tendinosis. That was a month ago. I am continuing to go to my physical therapist weekly and I started swimming at the local YMCA three times a week and practicing Tai Chi daily, which seems to help me as much as anything. Last August, when this all started, my PCP suggested that I take acetaminophen and Ibuprofen twice daily. I was doing that daily for nine months until reading your article about the risks of NSAIDs being contra-indicated for tendinosis.
I think your article is wonderful and has given me some concrete ideas about overcoming my handicap, tendinosis.