Few nutritional topics are as hotly debated as saturated fats. For the last 50 years, the guidance to limit them has been repeated so often it now feels ingrained.
Yet there’s a growing body of evidence refuting this advice. Some studies even show that saturated fats bring benefits, such as lower stroke risk. Fear of saturated fats may have been misplaced all along.
Most of the saturated-fat guidance dates back to the “diet–heart hypothesis” that dietary fat and cholesterol raise serum cholesterol, boosting heart-disease risk. Saturated fat was never actually proven to cause cardiovascular disease, but starting in the 1970s governmental nutrition policy responded to this hypothesis and recommended we limit fat intake.
Multiple recent peer-reviewed studies have found that diets high in refined carbohydrates and sugar — not saturated fat — are actually the culprits behind this epidemic of cardiovascular disease. Consider the following:
1. Blood-cholesterol levels do not tell the whole story.
Cholesterol is a waxy, fat-soluble substance transported throughout your body with carrier lipoproteins: low-density lipoprotein (LDL, or “bad cholesterol”) and high-density lipoprotein (HDL, or “good cholesterol”). These common nicknames, however, are oversimplified.
LDL cholesterol is not all bad, and lower isn’t always better. For example, one study showed that when LDL cholesterol drops below 70 mg/dL, the risk of hemorrhagic stroke increases.
Swapping saturated fat for mono- or polyunsaturated fat (such as olive or flaxseed oil) can lower your cholesterol and LDL. But evidence shows that this drop alone may not lower your risk of death from heart disease.
2. Unsaturated-fat sources vary in quality and health impact.
Polyunsaturated fats can come from omega-6 or omega-3 fatty acids. The surge in highly processed vegetable oils — corn, safflower, and soybean — in our foods has dramatically raised the ratio of poor-quality, pro-inflammatory omega-6 fatty acids to whole-food, anti-inflammatory omega-3 fatty acids in our diets. This can undermine our health.
3. Avoiding saturated fat can lead to increased carb intake.
Fat provides satiety, flavor, and “mouthfeel.” When we adopt low-fat diets or otherwise limit saturated fat in foods, we tend to add starch and sugar to improve taste.
4. Saturated fatty acids in the blood are not the same as dietary saturated fat.
Plasma saturated fat is closely tied with carb intake. Many of us can safely embrace full-fat yogurt, cheeses, grassfed red meat, and eggs, while limiting our consumption of refined carbs and sugars.
5. Genetics matter.
Genetically high cholesterol is often marked by inflammation and blood-pressure issues. Those who are predisposed to high cholesterol levels often respond well to moderating carbs instead of limiting saturated fats.
Still, there are people who may have a specific genetic variant that does make saturated-fat intake contribute more strongly to development of health issues. We do not all respond to food in the same way, and different approaches work for different people based on a variety of factors.
This article originally appeared as “Reconsidering Saturated Fats” in the June 2021 issue of Experience Life.


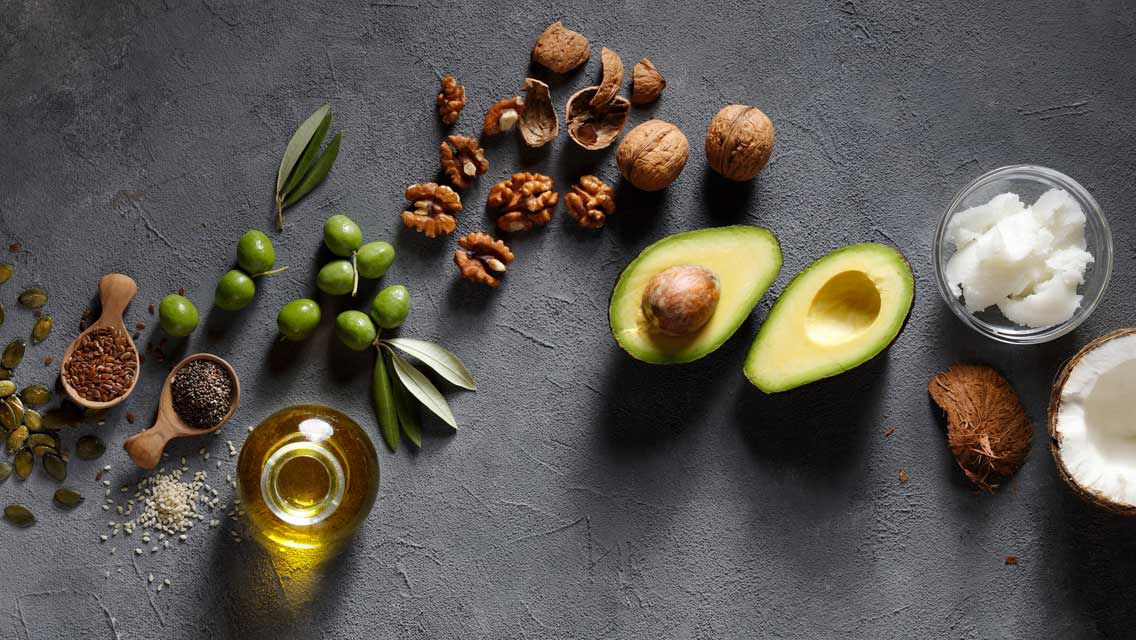


This Post Has 2 Comments
Genetics, meaning you like what your environment (parents) like because they liked it?
Semi good article but missing a lot of info on what foods; only categorized it. No sufficient details.