Temma Ehrenfeld had planned a perfect writers’ retreat: a house near the ocean, plenty of downtime, and healthy meals. But after a few days — and a few big bowls of the ratatouille she’d prepared — Ehrenfeld was so miserable with diarrhea and stomach cramps that she didn’t dare venture out to the beach on her breaks from writing.
To manage her irritable bowel syndrome, she’d been avoiding gluten for more than a decade, and she knew there was none in the food. So she blamed her digestive misery on the vegetables. When she returned home, she tried a low-FODMAP protocol, which restricts a number of common foods containing particular saccharides — natural sugars that can cause many people digestive distress.
Yet her symptoms persisted and multiplied. She began feeling itchy and congested, especially after one memorable meal of takeout fish, baba ghanoush, tomatoes, and salad dressed with balsamic vinegar. She decided to consult with nutritionist Tamara Freuman, MS, RD, CDN.
Freuman examined Ehrenfeld’s food journal and suggested a surprising diagnosis: histamine intolerance. She pointed to some of Ehrenfeld’s favorite foods, including the takeout fish, tomatoes, and vinegar, as potential triggers. All are high in histamines, or are histamine “liberators.”
Histamines are an organic chemical compound produced both within and outside the human body. They belong to a class of common amines that — along with tyramine in cheese and phenylethylamine in chocolate — can trigger food intolerances.
The immune system produces histamines to fend off allergens, but problems can develop if someone has difficulty processing the chemical, or if his or her body produces too much of it, says Minneapolis functional-medicine practitioner Gregory Plotnikoff, MD, MTS, FACP.
Studies suggest histamine intolerance occurs in about 1 percent of the population, though some experts believe that estimate is low. “Honestly, I think that’s just scratching the surface,” says Joseph Dizon, MD, chief of the Allergy and Immunology Department at Kaiser Permanente West Los Angeles Medical Center. He points out that allergists see cases every day.
Others agree with Dizon — and believe histamine intolerance may be increasing. “I’ve been in practice for about 30 years, and only in the last year or two have we begun to see a lot of histamine intolerance,” Plotnikoff says. “All of a sudden people are asking important new questions.”
Discover how histamines work to keep us healthy — and how they sometimes make us ill.
Too Much of a Good Thing
Histamines play a protective role in the body. They boost blood flow to areas affected by allergens and trigger sneezing, swelling, itching, wheezing, and other responses that help usher allergens out of the system. Still, they sometimes run amok, leading to a condition more accurately described as histamine overload, though “intolerance” remains the more common term.
Histamine intolerance is the body’s mishandling of the chemical, Dizon explains. This happens when the body produces too much of the compound or can’t break it down sufficiently. It’s why a case can mimic an allergic reaction: flushed face, itchy eyes, hives, or digestive woes.
A type of white blood cell called a mast cell produces histamine. These cells are key players in the immune system; Plotnikoff describes them as the body’s first responders.
Each mast cell contains several hundred chemicals, including histamine. If you get a cut, histamine sends extra blood to help flush harmful bacteria out of the wound. Likewise, if you encounter an allergen, mast cells bind to it and trigger the release of histamines as well as immunoglobulin E (IgE) antibodies. These prompt the usual symptoms of an allergic reaction. “Swelling, itching, runny nose, and watery eyes are classic examples of histamine in action,” Plotnikoff says.
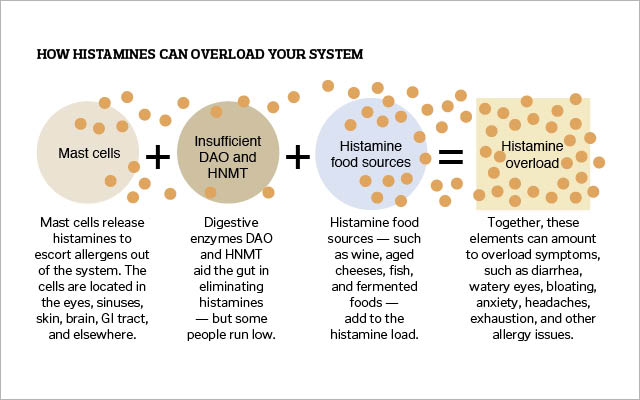
Mast cells are concentrated in areas of the body that are open to the outside world — the eyes, sinuses, skin, and urinary tract. But they’re active throughout the body, including the brain, where histamine acts as a neurotransmitter, and the gastrointestinal (GI) tract, where it plays a role in stomach-acid production.
Histamine affects so many different parts of the body that it makes an overload hard to track. “Histamine is all over the place,” Plotnikoff says. Unlike a simple urinary-tract infection or appendicitis, conditions in which just one system or organ is involved, histamine intolerance can create a range of symptoms throughout the body, including migraines, digestive troubles, and plain old allergy symptoms.
Overall gut health determines the body’s capacity to break down and eliminate histamines after they’ve done their work. Plotnikoff likens the gut to a sink’s plumbing. “What we don’t want is a clogged drain,” he says.
Two digestive enzymes that help the gut eliminate histamine are DAO (diamine oxidase) and HNMT (histamine N-methyltransferase). But they help some of us more than others. “There is great genetic variability among humans in how efficiently these enzymes work,” Plotnikoff points out.
We also vary in our capacity to produce them. DAO, which is created in the intestine, might be limited if there’s intestinal damage from leaky gut, Crohn’s disease, celiac, gluten intolerance, or SIBO (small intestinal bacterial overgrowth). Some foods — including alcohol, black and green tea, mate, and some energy drinks — also seem to block DAO.
Although the body makes its own histamine, it also receives it from food and other external sources. Certain beverages and foods, like wine and hard cheeses, are especially high in histamines, as is anything that’s pickled, smoked, fermented, or aged.
Leftovers are another potent source: Bacteria growing on food as it sits can produce histamine as a byproduct. (This was the problem with Ehrenfeld’s takeout fish — because fish is fairly delicate, it begins to decompose quickly after it’s cooked, and histamines accumulate.)
Then there are foods known as histamine liberators, such as tomatoes and strawberries. They don’t contain a lot of histamine but appear to trigger its release in the body.
Unlike classical allergies, histamine intolerance reacts in ways that are not usually consistent, even to the same food. You may be perfectly fine with a little cheese on your salad, for example, but could suffer a full-blown attack after eating a cheesy pizza served with a vinegary salad and glass of red wine. “Dose determines poison,” explains Plotnikoff.
Your system may also misidentify a food as an allergen and respond with a flood of histamines. “Sometimes the immune system can’t really ‘see’ all that well,” he says. “Every pollen has a license plate announcing, say, ‘I am ragweed pollen.’ But the license plate of a raw apple could look very much like ragweed,” causing the body to release histamine. A cooked apple won’t have the same effect.
A number of other factors can act as triggers, such as bacterial overgrowth in the intestines. And some people just have “rambunctious mast cells,” says Plotnikoff. This can lead to histamine overproduction along with other problems.
Histamine intolerance, like seasonal allergies, can strike at any point in life, even if there is no prior history of issues, according to registered dietitian Ginger Hultin, MS, RDN, CSO.
Reining in Runaway Histamine
Given all the factors involved in an overactive histamine response, it’s clear why identifying an intolerance is often tricky. The lab testing is complex and the range of reactions is vast: diarrhea, watery eyes, bloating, anxiety, headaches, and exhaustion, along with other common allergy symptoms. And the symptoms themselves are often oblique. A flushed face after drinking red wine, for example, could be a sign of a histamine intolerance — or any number of other things, says Plotnikoff.
“It’s hard because the symptoms can be a little bit vague,” agrees Hultin. She stresses the importance of a full health workup to avoid mistaking other issues for histamine intolerance. She also suggests closely tracking food intake to detect whether histamines might be the problem.
To identify whether histamines might be causing you trouble, and to treat issues related to overload, providers recommend the following:
- Keep a food journal. Keep close tabs on your diet with a food journal to suss out what’s triggering symptoms, Plotnikoff advises.
“A food journal asks people to pay close attention to both their diet and their experience of symptoms, and that heightened awareness often leads to a lot of insights,” he says. “Life goes by in a blur, but recording foods and how your body responds can actually be a mindfulness exercise. I think the goal is awareness. I strongly believe that awareness unleashes one’s inner wisdom.” (For more on this, read “The Mindful Food Journal.”) - Eliminate high-histamine foods. Next, you can experiment with eliminating certain foods and tracking your symptoms (or their disappearance), then reintroducing the foods. Although you can do this on your own, Hultin says, it may be helpful to partner with a professional, especially because eliminating all foods high in histamine could become overly restrictive.
“I’d hate for someone to pull themselves off these healthy foods [like tomatoes and strawberries] if the root cause is actually something like dehydration,” she explains.
Whereas diseases such as celiac can be managed by avoiding a single ingredient, handling histamine intolerance is rarely as simple as avoiding one food — or even a list of foods. Because histamine is essential to so many functions in the body, it’s impossible to avoid it all together.
So, although patients find varying degrees of success by ingesting less histamine, Plotnikoff says, a low-histamine diet is best employed as part of an overall treatment plan to help manage an overactive immune system. This includes reducing histamine triggers, supporting healthy enzyme function, and treating any underlying causes — like leaky gut — that might be exacerbating the problem.
As with any systemic health issue, the most important ingredient in detection and recovery is patience. Ehrenfeld, for instance, still hasn’t solved all of her food issues, but she has found that avoiding high-histamine foods — especially in combination with each other — allows her to get out the door and function again. And that is a pretty good place to start.
 |
|
Foods to Track If You Suspect a Histamine Intolerance
Some foods are naturally high in histamines; others — like cured and smoked foods — produce them as they’re prepared. Functional physician Gregory Plotnikoff, MD, created this “rough guide” to histamine foods, though he emphasizes the great variability in how people react to individual items. If you suspect histamines are causing allergy-like symptoms, keep an eye on your reaction to the following.
Histamine-Releasing Foods
- Shellfish
- Nuts
- Black and green tea
- Spinach
- Avocado
- Eggplant
- Vinegar
- Mustard
- Olives and pickles
- Some fruits, including citrus, strawberries, cherries, raspberries, bananas, pineapple, and dried fruits
Histamine-Rich Foods
- Leftovers, especially leftover meats
- Aged cheeses
- Fermented foods, including yogurt, sauerkraut, soy sauce, kefir, kombucha, and others
- Fish, especially fish that is not extremely fresh
- Cured meats, including bacon, salami, pepperoni, luncheon meats, sausages, hot dogs, and others
- Tomatoes, including ketchup
- Chocolate
DAO-Blocking Foods
- Alcohol
- Energy drinks
- Tea, including black, green, and mate
This originally appeared as “The Trouble With Histamines” in the May 2019 print issue of Experience Life.




This Post Has 0 Comments