Our bodies are designed to digest food. So why do so many of us suffer from digestive distress?
An estimated one in four Americans suffers from gastrointestinal (GI) and digestive maladies, according to the International Foundation for Functional Gastrointestinal Disorders. Upper- and lower- GI symptoms, including heartburn, dyspepsia, irritable bowel syndrome, constipation, and diarrhea, represent about 40 percent of the GI conditions for which we seek care.
When flare-ups occur, antacids are the go-to solution for many. Proton pump inhibitors (PPIs) — one of the most popular classes of drugs in the United States — and H2 blockers both reduce the production of stomach acid and are commonly prescribed for chronic conditions.
These medications may offer temporary relief, but they often mask the underlying causes of digestive distress and can actually make some problems worse. Frequent heartburn, for example, could signal an ulcer, hernia, or gastroesophageal reflux disease (GERD), all of which could be exacerbated rather than helped by long-term antacid use. (For more on problems with these medications, see “The Problem With Acid-Blocking Drugs.”)
Research suggests a link between chronic PPI use and many digestive issues, including PPI-associated pneumonia and hypochlorhydria — a condition characterized by too-low levels of hydrochloric acid (HCl) in gastric secretions. A shortage of HCl can cause bacterial overgrowth, inhibit nutrient absorption, and lead to iron-deficiency anemia.
The bigger issue:
As we attempt to suppress the symptoms of our digestive problems, we ignore the underlying causes (typically lifestyle factors like diet, stress, and sleep deficiency). The quick fixes not only fail to solve the problem, they can actually interfere with the building and maintenance of a functional digestive system.
When working optimally, our digestive system employs myriad chemical and biological processes — including the well-timed release of naturally produced digestive enzymes within the GI tract — that help break down our food into nutrients. Digestive distress may be less a sign that there is excess acid in the system, but rather that digestive-enzyme function has been compromised.
For many people with GI dysfunction, supplementing with over-the-counter digestive enzymes, while also seeking to resolve the underlying causes of distress, can provide foundational support for digestion while healing takes place.
“Digestive enzymes can be a big help for some people,” says Gregory Plotnikoff, MD, MTS, FACP, an integrative internal-medicine physician and coauthor of Trust Your Gut. He cautions that supplements are not a “fix” to rely on indefinitely, however. Once your digestive process has been restored, supplements should be used only on an occasional, as-needed basis.
“When we are in a state of reasonable balance, supplemental enzymes are not likely to be needed, as the body will naturally return to producing them on its own,” Plotnikoff says.
Read on to learn how digestive enzymes work and what to do if you suspect a digestive-enzyme problem.
Breaking It Down
Digestive enzymes are proteins our bodies release in order to chemically disassemble the food we eat and allow the body to absorb all of its component nutrients. Regardless of how much nourishment we take in, our bodies can’t access the nutrients required for optimal health and energy without sufficient digestive-enzyme production.
From the moment we begin eating, digestive enzymes get to work. Different enzymes break down different components of our food at various points along its journey through our gastrointestinal system.
Food first encounters salivary amylase in the mouth, where the enzyme begins turning starches into sugars. When we chew our food thoroughly, we create smaller particles with a greater resultant surface area, allowing enzymes more efficient access to the contents.
In the stomach, our chewed-up food (called bolus) comes into contact with gastric juices, which include hydrochloric acid (HCl — a corrosive liquid that further breaks down food and helps kill any lingering pathogens) and pepsin (an enzyme that digests proteins found in meat, dairy, eggs, and seeds).
As the partially digested food, now called chyme, is released from the stomach into the duodenum (the first section of the up-to-25-foot-long small intestine) it encounters more enzymes. Pancreatic amylase converts starch into sugars; pancreatic lipase breaks down fat; and activated trypsin continues to break down protein. Bile, a digestive fluid released by the liver (by way of the gallbladder), emulsifies fat here, too.
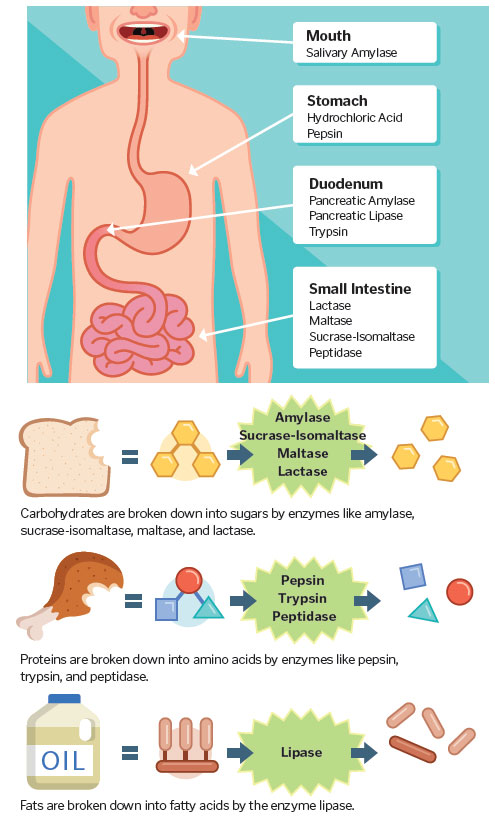
Even the walls of the small intestine release digestive enzymes. The brush border (millions of fingerlike protuberances called villi that line the interior of the small intestine) houses lactase, maltase, and sucrase-isomaltase, plus peptidase, enzymes that complete the digestion of your food and enable absorption of the nutrients into your small intestine.
Anything that’s not absorbed by this point in the process is either excreted or recycled. (For more on that process, see “Fiber: Why It Matters More Than You Think.”)
The Stress Factor
Your digestive challenges may or may not be directly related to what you are eating, says integrative internal-medicine physician Gregory Plotnikoff, MD. Because the neuroendocrine system regulates digestion, he explains, any kind of stress can alter its function.
Here are five major stress sources that Plotnikoff says can affect your digestion, nutrient absorption, and more:
- Environmental stress results from exposure to toxic factors that can disrupt gut ecology. These include hazardous chemicals in -pesticides, herbicides, parabens, and antibacterial compounds such as triclosan.
- Physical stress from overexertion, chronic illness, surgery, inadequate sleep, and disrupted daily rhythms (all-nighters, traveling across time zones) can undermine digestive processes.
- Emotional stress pumps up stress-hormone production and can, in turn, excessively increase or decrease stomach-acid production. Getting stuck in fight-or-flight mode slows digestion and the production of digestive enzymes.
- Pharmaceutical stress from the ongoing use of antacids, antibiotics, chemotherapy drugs, and steroids can interfere with gut ecology, which can adversely affect digestion.
- Dietary stress can result from food allergies, intolerances, and sensitivities. Those whose symptoms are delayed after being exposed to certain foods may not recognize their connection with digestive troubles.
Is It An Enzyme Deficiency or Something Else?
Digestive distress can occur as the result of various food-based or physiological factors, says Thomas Sult, MD, a functional-medicine physician and author of Just Be Well. For those who want to investigate the likely causes of their digestive distress, Sult advises the following steps:
1. Watch the clock. If you feel bloated within 10 minutes of eating, it’s likely a hydrochloric-acid (HCl) insufficiency.
If you experience gas or bloating, or you feel like your food is just sitting in your stomach 30 to 60 minutes after eating, there’s a good chance your natural digestive enzymes aren’t doing their job and you could benefit from supplementation. Another indication of digestive-enzyme deficiency is undigested food particles in your stool, or floating or oily stools.
If your symptoms start one to three hours after eating, it’s more likely a small-intestine issue, such as small-intestine bacterial overgrowth (SIBO).
2. Get tested. A simple stool test can confirm enzyme and HCl deficiencies. It can also reveal bacterial and fungal imbalances and help identify other factors that may be throwing your digestion off track. From there, you’ll need to work with your practitioner to test out recommended treatment approaches. (See next page for an overview of how conventional and progressive strategies differ.)
Sult recommends getting your stool sample evaluated if you regularly experience any of the symptoms above, or suffer from unexplained weakness and low energy and don’t get relief from taking supplemental enzymes or HCl.
If you experience more severe symptoms — such as blood in the stool, weight loss, anemia, increased fatigue, or pain during or immediately after eating — see your healthcare practitioner immediately for further evaluation.
Enzyme Essentials
Here’s what you need to know before hitting the supplement aisle. If you’re taking other medications, consult first with your doctor or pharmacist.
- Keep it simple. Unless you’ve been advised otherwise by a nutrition or medical pro, start with a high-quality “broad spectrum” blend of enzymes that support the entire digestive process, says Kathie Swift, MS, RDN, education director for Food As Medicine at the Center for Mind-Body Medicine. “They cast the widest net,” she explains. If you find these aren’t helping, your practitioner may recommend enzymes that offer more targeted support.
- Start slow. Determining proper dosage may take some experimentation, Swift notes. She recommends starting with one capsule per meal and taking it with water just before you begin eating, or at the beginning of a meal. Observe results for three days before increasing the dose. If you aren’t seeing results from two or three capsules, you probably need to try a different strategy, such as HCl supplementation or an elimination diet.
- Don’t expect a cure-all. “I have the same issue with long-term use of digestive enzymes that I have with popping PPIs,” says Plotnikoff. “If you’re taking them so you can have massive amounts of pizza or beer, you are not addressing the driving forces behind your symptoms.”
A Better Path to Digestive Health
For too many people, fighting the symptoms of digestive distress becomes a way of life. But it doesn’t have to be that way. Here are two contrasting scenarios: the conventional-medical approach and the more progressive strategy embraced by many integrative and functional-medicine practitioners. Which do you prefer?
The Conventional Path
- Heartburn and reflux lead to regular use of over-the-counter antacids.
- Antacids begin to lose their effectiveness. Doctor prescribes a proton pump inhibitor (PPI). Symptoms initially subside but then begin to recur.
- Doctor recommends an endoscopy, which reveals redness and inflammation.
- Digestive issues and medication side effects begin to affect eating and sleep patterns.
- Stress levels rise, making indigestion worse and negatively affecting overall well-being.
- Cycle continues, with escalating attempts to manage with medication.
The Progressive Path
- Chronic heartburn and reflux lead to consultation with digestive-health expert.
- After detailed evaluation, practitioner suspects inadequate digestive action and prescribes a stool test to clarify root causes.
- Practitioner confirms low stomach-acid and enzyme levels are interfering with proper digestion.
- Practitioner recommends digestive enzymes and HCl supplements along with dietary adjustments.
- Supplements ease chronic symptoms; physician suggests additional dietary refinements and stress-reduction techniques.
- Over time, digestive balance is restored; supplements can be used on an as-needed basis.
Download the “A Better Path to Digestive Health” PDF.
This originally appeared at “Digestive Enzymes.”




This Post Has 2 Comments
What are some good foods to eat (versus supplements) to address gas and bloating?
How can I get off of PPIs? They are compromising my microbiome and my bone health. I have rampant reflux — I’ve seen it bubble back up into my esophagus in real time on an esophagram.