Many of us focus more on how our feet appear on the outside than what might be going on inside — and there is a lot going on.
Each foot is home to 33 joints, 26 bones, and more than 100 muscles, tendons, and ligaments encased by thick connective tissue called fascia. Despite their complexity and essential role in our mobility, our feet get surprisingly little attention — until a problem surfaces, that is.
Foot issues are often painful: Flat arches, bunions, plantar fasciitis, and arthritis are just a few common complaints. As we age, these conditions can have a debilitating effect on our quality of life.
“Foot pain can erode our overall health and well-being,” says Paul Langer, DPM, board-certified podiatrist at Twin Cities Orthopedics and an American Academy of Podiatric Sports Medicine fellow. That’s because foot complaints are never isolated in the feet — they can cause, or be caused by, issues elsewhere in the body. Once foot pain sets in, it can limit mobility and contribute to a sedentary lifestyle, which is associated with many chronic illnesses.
The cycle is vicious but preventable. When foot problems arise, however, we usually try to treat them from the outside in, with special ointments, complex orthotics, and technologically advanced socks. Or, worse, we ignore them altogether and cross our fingers that they will resolve themselves.
But there is a better way. By focusing on the fitness of our feet, including their strength and mobility, we can reclaim our foot health and prevent further issues. Fit feet contribute to full-body fitness, and a little TLC for your foundation can dramatically improve how the rest of your body feels and functions.
Everything’s Connected
Remember the old spiritual “Dem Bones,” about the toe bone connecting to the foot bone, and so on up the body? This song tidily describes what is known as the kinetic chain — the integration of not just bones but also joints, nerves, and muscles that work together to move the body.
Because humans evolved as a species that stands upright, the feet are the body’s foundations at the base of the kinetic chain. They are connected to the rest of the limbs and allow us to walk, run, and play.
“A lot of people think the foot acts as an independent unit, but it affects a lot of things upstream as well,” says Mike Gauvreau, MPT, a performance physiotherapist in Ottawa, Canada.
The foot contains so-called intrinsic muscles, which connect all the bones within, including the ankle. Extrinsic muscles attach the feet to the lower leg, which connects to the knees, hips, back, neck, and beyond.
The intrinsic muscles within the feet and the higher-chain extrinsic muscles both play a role in foot and ankle motion, including rotation and stabilization.
When any of these muscles are weak, it throws off your biomechanics. This affects shock absorption and contributes to pain and weakness all the way up the kinetic chain, explains Erika Mundinger, DPT, OCS, a physical therapist in St. Paul, Minn.
The reverse is also true: Weakness in other parts of the body can indicate trouble in the feet.
Poor posture, for instance, may mean your toe flexors are not strong enough. Additionally — and unexpectedly — blood pressure, body composition, and exercise and sleep habits were linked to toe-flexor strength in a 2017 study published in the Journal of Foot and Ankle Research.
When your toe flexors are strong, you’re likely more active — and that helps counteract other health issues. Additionally, health problems and poor habits can directly affect the health of your feet. And when foot health deteriorates, so can mobility and quality of life.
In other words, the feet are an integral part of any bodywide wellness program.
Consider your arches: They are supported by three muscles and the plantar fascia, a thick band of tissue running along the foot bottom that connects your heels to your toes. When you lift your foot to walk or run, these muscles and the plantar fascia tighten and pull on the arch to “wind up.” As you return your foot to the ground, they stretch and the arch flattens. Some of the energy from the wind-up continues pulling the forefoot toward the heel, keeping the arch slightly rounded to absorb the shock.
As part of a kinetic chain that connects the feet’s intrinsic muscles to extrinsic muscles up into the hips, weak or flat arches may not be the problem; instead, they often signal weak hips, says Mundinger.
The hips are important ball-and-socket joints that can produce rotational force, explains Gauvreau. If you lack hip strength and stability, your knees and feet may draw inward because of lack of control, thereby taking on excess stress. What’s more, if your hips — which include the glutes — are weak or underused, your feet have difficulty maintaining an ideal position when you walk or run. So, you might be better off strengthening your side-butt muscles (the gluteus medius and minimus) than investing in orthotics.
Regardless of whether your foot pain stems from a job that keeps you on your feet all day or chronic health issues, everyone can benefit from giving their feet a little more thought and attention.
Fit Feet Qs
Life isn’t easy on our feet. We use them and abuse them, and they end up sore. These questions can help you pinpoint the source of your foot issues, and the solutions offer a common thread: strength training.
Are you getting older?
This is a trick question. We’re all aging, which means our foot mobility will eventually begin to degrade, if we don’t work on it. We begin to lose soft-tissue elasticity and joint range of motion at a rate of about 1 percent per year starting at age 25, says podiatrist Paul Langer. This means by the time we reach 50, we’ve lost 25 percent.
The Path to Fit Feet:
Strength training can keep your feet limber and improve mobility; turn to page 64 for tips. Simple stretches also help (learn more: Fitness Fix: Tight, Sore Feet).
Do you have chronic health issues?
Persistent pain, swelling, and stiffness in your feet may be a sign of rheumatoid arthritis, an autoimmune disorder. Many people suffer from gout, another form of arthritis that’s characterized by sudden and intense joint pain and swelling, typically at the joint of the big toe. Some people with type 2 diabetes develop diabetic neuropathy, a type of nerve damage that can begin with burning, tingling, weakness, or pain in the legs and feet, and eventually lead to numbness.
The Path to Fit Feet:
Build up your strength and restore blood flow with gentle movement to counteract inflammation and the effects of arthritis.
Are your feet tired at the end of a long day?
Whether you sit or stand all day, repeated sedentary activity will reduce circulation, which can cause swelling and fatigue in your feet.
The Path to Fit Feet:
Stretching throughout the day and regular strength training will help with everyday endurance, while wearing supportive footwear can also make a difference (see Choosing the Best Shoe above).
Are you pregnant — or have you had children?
Hormonal changes during pregnancy can result in increased elasticity of the ligaments, which can cause the feet to grow in size. Weight gain, too, can prompt swelling, and cause a size increase. After childbirth, many women report that their old shoes no longer fit.
The Path to Fit Feet:
Strength training can help your feet regain stability and structural integrity, and it can alleviate lingering swelling by improving circulation. A mindset shift — as well as new shoes, per our guide at right — can help you accept the new shape of your feet.
Do you have soreness in your knees, hips, or back?
Your foot bones are connected to all other bones, muscles, and fascia, particularly through the lower body. Weakness in the knees, hips, and lower back doesn’t always mean that the problem is located in that specific spot. In fact, weakness in the feet can wreak havoc throughout the kinetic chain.
The Path to Fit Feet:
Strength training, with a focus on the lower body, including the feet, may ease many structural pains.
Strength Training for Your Feet
Start your journey to fitter feet by practicing regular strength and mobility exercises that target your feet, ankles, hips, and core. You can prehabilitate your feet to prevent injury or offset age-related issues. “You don’t have to give up and think, I’m too old to fix it,” says Eischens Yoga teacher Lynn Shuck. “You’re not.”
There are a handful of simple strength and mobility drills you can practice to keep your feet healthy. For example, one easy way to create greater joint mobility and counteract all the time you spend in shoes is to roll the soles of your bare feet over a tennis ball periodically throughout the day, she says. If your feet are especially tight and tender, begin in a seated position. If your feet aren’t as tense, you can roll each foot while standing or even switch to a smaller ball, such as a handball.
Mindful walking helps build awareness of how you’re using your feet, while also developing foot strength and mobility, says performance physiotherapist Mike Gauvreau. Find an area where you can walk barefoot (you can also wear minimalist shoes) and spend 10 to 15 minutes walking — paying close attention to how you’re naturally placing your feet. (Learn more about your gait at Relearn to Walk.)
Finally, building full-body strength will go a long way toward prehabbing and rehabbing foot conditions. “All of the muscles and joints of the lower limb are involved in foot and arch support, and thus it’s important to make sure we’re strengthening all of them,” explains physical therapist Erika Mundinger, who designed the following routine.
5 Steps to Strong Feet
Perform this routine two or three times per week, preferably before workouts.
Note: If you have moderate foot pain that doesn’t improve after two weeks, consult a physical therapist or podiatrist about targeted treatment. If you can’t walk without limping or you suffer from acute foot pain and swelling, seek professional help before beginning this program.
1) Dead Bug
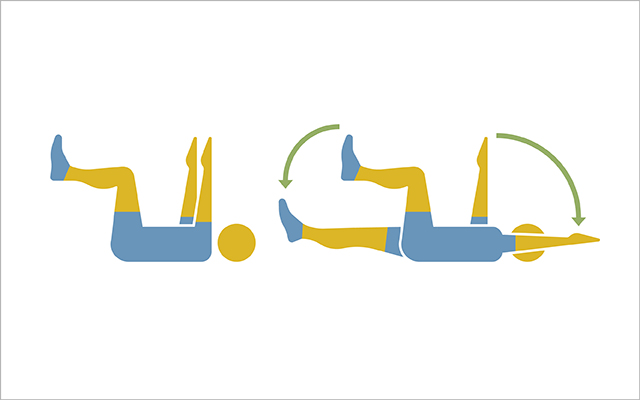
This move teaches you how to stabilize your pelvis and spine while moving your limbs, which is key for optimal posture, explains Mundinger. When your posture is stable, your feet can land in a better position.
- While lying down with knees bent, press your lower back into the floor and then lift both knees until your shins are parallel to the floor. Reach your arms toward the ceiling.
- Tighten your abdominals, then lower one arm toward the floor alongside your ear while simultaneously straightening the opposite leg. Lower your limbs only as far as you can without arching your lower back.
- Return to start and repeat with the opposite arm and leg. Complete three sets of 10 reps per side.
2) Hip Thrust

This exercise strengthens your gluteus maximus and hamstrings. When these muscles are strong, they stabilize your thighbones better, keeping your knees and feet from rotating in or out as you walk or run.
- Position your body so your upper back is resting against a bench or box, with your knees and hips bent.
- Tighten your abdominal and gluteal muscles and push through your feet to lift your hips until they’re parallel to the floor. Do not arch your back during the exercise.
- Hold briefly, then lower your hips to start. Repeat to complete three sets of 10 reps. Make the exercise harder by adding weight across your hips.
3) Banded Sidestep
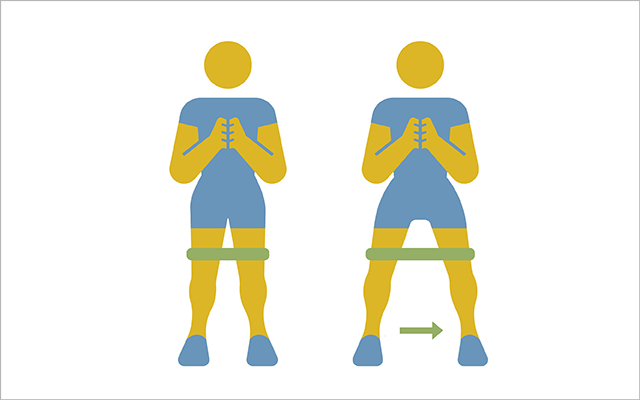
This works both your gluteus maximus and medius, which minimizes rotation of your thighs and ankles.
- Loop a resistance band around your legs just above the knees and lower into a quarter-squat. You should feel mild to moderate tension in the band.
- With your arms in front of you, step one foot to the side. Follow with the opposite foot. Continue for 10 reps in one direction, then repeat in the opposite direction.
- Tighten your core as you sidestep to avoid rocking motions. Complete three sets of 10 reps per side.
4) Seated Towel Pickup
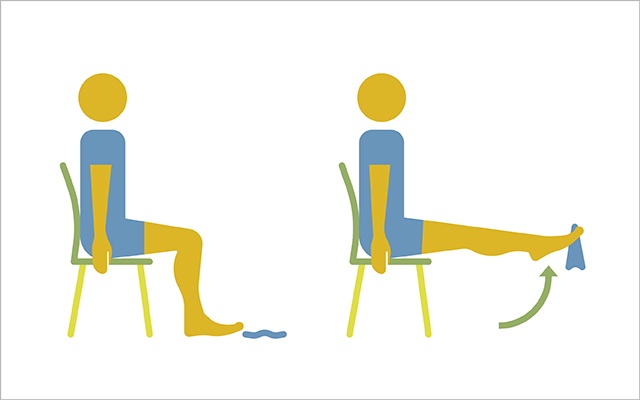
This exercise strengthens your foot arch to help prevent pronation or arch collapse.
- Sit in a chair with a towel on the floor in front of you.
- Using just your toes, pick up the towel, then drop it, and pick it up again.
- Keep your movements slow and controlled. Complete three sets of 10 reps per foot.
5) Single-Leg Balance on Foam Pad
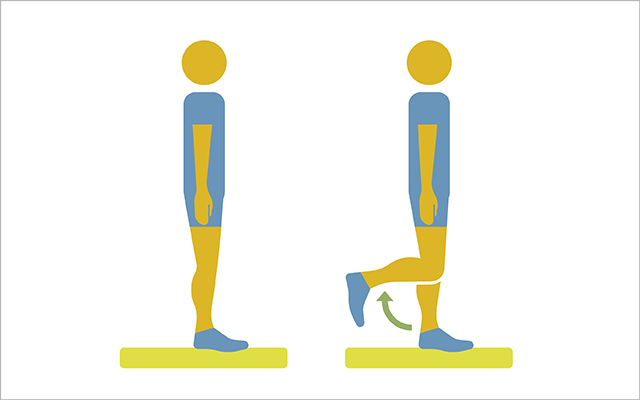
This exercise activates all the muscles in your legs and core to limit rotation of your hips, knees, and ankles, while also strengthening your arch and all the intrinsic muscles of your feet.
- Standing on a foam pad, bend one knee 90 degrees to lift your foot behind you, balancing on your standing leg. Keep your thigh, glutes, and core activated, and don’t let your legs touch while you balance. Hold for several seconds before lowering your foot.
- Complete three sets of 10 reps per leg.
How to Choose the Best Shoes
Cultures that routinely wear shoes have higher incidences of foot deformities and pain than cultures that go barefoot, says podiatrist Paul Langer. In an ideal world, we’d all be safe and comfortable walking around barefoot all the time, he says. And while there are some ways to increase time without shoes, very few of us can reasonably give them up completely. With that reality in mind, here are some of our experts’ top tips for minimizing the adverse effects of shoes.
Beware of lifted heels. Many shoes, including running shoes, are designed to prop your heel up. “It’s like you’re standing on a ramp,” explains performance physiotherapist Mike Gauvreau, and it ultimately changes the way you move.
High heels and even athletic shoes with a lift, such as supportive sneakers and weightlifting shoes, place your ankles and calves in a shortened position, ultimately creating more tension. This can cause trouble with extended use. Save dress shoes with higher heels for special occasions, and limit the use of athletic shoes with a lift by mixing in lower- and no-heeled sneakers.
Steer clear of flip-flops. “Shoes that make your foot hold on — instead of the shoe holding on to your foot — create tight, stiff feet,” says Lynn Shuck, an Eischens Yoga teacher based in Minneapolis. This can result in plantar fasciitis, tight hamstrings, and back pain, among other issues. Choose shoes that have a secure heel strap or well-fitting enclosed heel.
Avoid crowding your toes. Many shoes are too narrow — especially in the toe box — and compress your tarsal and metatarsal bones (the toes and the bones in your forefoot). If you compress your feet long enough, your mobility becomes limited, says Shuck. “If I’d worn gloves on my hands for 50-plus years, they wouldn’t move much. That’s what we’ve done with our feet.” Again, high heels and dress shoes are often the culprits, if they have a narrow toe box. Look for shoes with ample width so your toes can flex.
Don’t go soft. Shoes are often packed with cushioning, which actually weakens your feet over time, and the lack of sensory feedback alters your walking mechanics. Every time your foot hits the ground, it receives signals from the ground via nerve fibers. If you’re wearing shoes with thick padding, your feet need to land harder to pick up that feedback, and you’ll be less mindful of how you’re interacting with the ground. But if your feet are minimally cushioned, you’ll be more aware of how you’re walking. “You’ll wind up walking more naturally and efficiently,” Gauvreau says.
Avoid the quick fix. Runners are especially susceptible to developing pain as a result of their footwear. Interestingly, research suggests that the best way to minimize your risk of foot pain and injury is to choose running shoes based on comfort, as opposed to shoes that “fix” a biomechanical problem.
Runners may be familiar with this scenario: You visit a running store to have your gait assessed. The assessor determines your degree of pronation, or how far your foot rolls inward with each step. If you’re an overpronator, you land on the inside of your foot; if you’re an underpronator, you land on the outside. Neutral pronators land in the middle. The salesperson will recommend a shoe to resolve it, thus helping you avoid injury.
Sounds reasonable, but research has shown that this approach has no effect on injury prevention. A 2015 study of running injuries found no conclusive evidence that pronation had any effect on running-related injuries. Instead, the research authors suggest two alternative models for selecting shoes to mitigate injury risk: the comfort filter and the preferred movement pattern.
Choosing a shoe based on comfort will enable you to maintain your preferred movement pattern, reducing the risk of injury, a model first proposed by biomechanics expert and lead study author Benno Nigg, PhD.
“Our movement patterns are as unique as our signature,” explains Langer, “and anything that causes us to deviate from our preferred movement pattern will cause us to work harder, be less metabolically efficient, fatigue sooner, and increase our risk of injury.”
If you are free of foot pain, he recommends choosing running shoes based on what feels right: “Since comfort and movement patterns are very complex and can’t be measured, we recommend that people try shoes on, make comparisons, and then select the most comfortable shoe.”
This originally appeared as “Best Foot Forward” in the January/February 2019 print issue of Experience Life.




This Post Has 0 Comments